Launch event report by Anne Marie Matarrese, Chair of Derbyshire Maternity and Neonatal Voices Partnership
On Monday 15 of May 2023, I attended the launch in parliament of the Saving Babies’ Lives Progress Report, by the Sands and Tommy’s Joint Policy Unit. The event was hosted by Olivia Blake and Cherilyn Mackrory, both MPs who have bravely shared their own stories of loss and work to raise awareness on this issue and drive improvements.
Saving Babies’ Lives Progress Report, by the Sands and Tommy’s Joint Policy Unit. The event was hosted by Olivia Blake and Cherilyn Mackrory, both MPs who have bravely shared their own stories of loss and work to raise awareness on this issue and drive improvements.
The event was attended by many MPs, as well as the Health Minister Maria Caulfield, representatives from national charities and organisations, as well as the Royal College of Midwives and Donna Ockenden. Many of those who spoke, from MPs to midwives, were bereaved parents themselves, with very different experiences of care. Hearing their stories in this context was a very powerful moment.
“There is a risk of going backwards”
Sadly the progress report highlights some worrying data. Overall, we are not on track to meet the ambition of reducing stillbirth and neonatal deaths by half in England by 2025. Interim targets to reduce deaths by 20% were met in 2020 but, rates have increased again in 2021.
On neonatal deaths specifically, not enough progress has been made and there has been no change in pre-term births since 2010. There is also no data on miscarriage, making it impossible to monitor the impact of policy change.
Research
The cause of death still remains unknown for 33% of stillbirths and 7% of neonatal deaths, with 1 out of every 5 potentially avoidable. The impact of this on bereaved families cannot be underestimated, with MP Cherilyn Mackrory asking, “How can you recover when you don’t know why your baby died? We need more research, more neonatal pathologists, proper investigations, lessons learned without fear and adequate support for midwives.” Soberingly, for every £1 spent on maternity, only 1p is spent on pregnancy research, which is far below other health care research spends (with 12p going towards research on heart disease, for instance).
Safety and systemic issues in maternity and neonatal services
The report also points out the declining safety and quality ratings at Trusts nationally and acknowledges that systemic issues in maternity and neonatal services need to be addressed. “Some midwives have told me it has been 5 years since they worked a shift with the right number of midwives on the unit” said Olivia Blake MP. The report identifies a number of key themes and how these impact safety, including engagement with service users, stating that there are ‘persistent issues around women and birthing people not being listened to’, despite policy initiatives introduced to improve the safety of maternity care in England. All agreed that safe staffing levels and support for midwives were key elements.
Addressing disparities
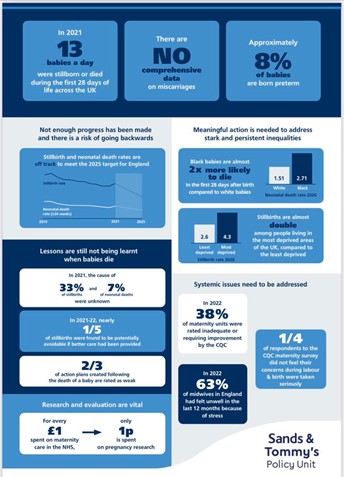 Stillbirths, neonatal deaths and preterm births remain more common among babies from minoritised ethnic groups, with black ethnicity also associated with a 43% higher risk of miscarriage compared to white ethnicity. Stillbirth rates are almost 2 times higher among those living in the most deprived areas, compared to the least deprived.
Stillbirths, neonatal deaths and preterm births remain more common among babies from minoritised ethnic groups, with black ethnicity also associated with a 43% higher risk of miscarriage compared to white ethnicity. Stillbirth rates are almost 2 times higher among those living in the most deprived areas, compared to the least deprived.
At the event we heard from Alicia Burnett, Tommy’s midwife and founder of Black Baby Loss Awareness Week. Alicia shared her story of loss and her work to ensure every woman, birthing person and parent receives the care they need. Streatham MP Bell Ribeiro-Addy also reflected on institutional racism, how this affects families, and the importance of listening to women, “So much would be resolved if we did”, concluded the MP.
Learning from families
More needs to be done to truly listen to families and learn from their experience, “..it has become mandatory for the NHS to review the death of a baby, but there are still many barriers to full and transparent reviews”, said Charlotte Bevan, SANDS, “Hospitals sometimes fail to honestly evaluate. Not listening to parents is a missed opportunity to learn. We are getting better but families are still suffering. The system, its culture and process hinder health care providers to support and learn from practice”, she added.
Maria Caulfield, the Health Minister, spoke about how baby and pregnancy loss is a significant priority for the government, adding that “the government is listening, women are being heard. We can make a significant difference in a short time through funding, research and better support.”
Looking forward
The event was clearly a very important opportunity to raise awareness amongst policymakers and the report will certainly be a powerful tool, bringing together the most recent data and recommendations to advocate for change.
As a service user and a bereaved parent myself, I still have many questions, and concerns, particularly with the rising number of deaths. Version 3 of the Saving Babies Lives Care Bundle, the guidance produced by the NHS to help reduce perinatal mortality across England will also soon be launched. The previous versions have had profound effects, such as helping to reduce the proportion of women recorded as smoking at delivery (down to 11.8%) and increasing the detection of small for gestational age (SGA) babies (up to 54%). It has also affected the rate of interventions, with increases in inductions of labour (by 19.4%) and emergency caesarean births (by 9.5%).
While Version 2 of the Care Bundle did seek to address this increase by focusing more attention on those at highest risk of stillbirth or pre-term birth, what progress has been made on this? As a service user I would also like to know how the impact of this guidance on women and birthing people’s experience of labour and birth has been monitored. The guidance does talk about the importance of personalised care and choice, but how effective is this? Nationally, and on a regional level, I feel there is still a lot of work to be done on ensuring that more women and birthing people truly feel listened to, have supportive conversations with their health care providers and are provided with enough information on the benefits and risks of each option. I am hopeful that Maternity and Neonatal Voices Partnerships around the country can play a key role in helping to make this happen.
By Anne Marie Matarrese, Chair of Derbyshire Maternity and Neonatal Voices Partnership @DerbysMNVP
Further resources
- Saving Babies Lives 2023 Full Progress Report
- Information about Saving Babies Lives Care Bundle from: Tommy’s / NHS
- Patient Information Forum Maternity Decisions Report, Induction Survey Summary (2021)
